Accelerators for Health and Medicine
Accelerators for Health and Medicine
The most direct way that particle accelerators impact most of our lives will be through their applications in medicine. With the advancement of accelerator science, new techniques for the treatment of cancer and diagnosis of various diseases have contributed significantly to major steps forward in the last decades.
Treating Cancer
One of the most important of all applications of particle accelerators is their application in the treatment of cancer. Cancer takes on many forms, so the treatment for cancer must also take on many forms. The main types of cancer treatment are:
- surgery, where the cancerous tissue is surgically removed,
- chemotherapy, where powerful cancer-killing medicine is given to the patient,
- radiotherapy, where the cancer is destroyed by energy deposited by radiation.
Accelerator based treatments fall into the category of radiation therapy. Presently about 50% of all patients with cancer will undergo radiation therapy often in conjunction with other treatments such as chemotherapy or surgery. The most common form of radiation therapy is external beam radiotherapy where a beam of radiation is fired into the body by a particle accelerator. The different types of radiation used are discussed below.
X-Ray therapy
X-ray therapy is the most common form of radiotherapy. High energy X-rays - generated by firing electrons at a material like tungsten - are directed into a cancerous tumour. The radiation damages the DNA of the cancerous cells which ‘kills’ the cells. A high dose in the tumour is essential in the curing process by radiation. Unfortunately the X-ray radiation doesn’t only harm the cancerous cells; it also damages healthy cells at locations in the patient’s body that cannot be avoided by the X-ray beam. This can lead to unpleasant side effects for the patient such as pneumonitis, dry mouth due to loss of saliva production and damage to the skin. The aim of all new techniques in radiotherapy is to deliver a high dose of radiation to the tumour (to get a high cure rate) whilst reducing the radiation dose in healthy tissue (to reduce side effects).
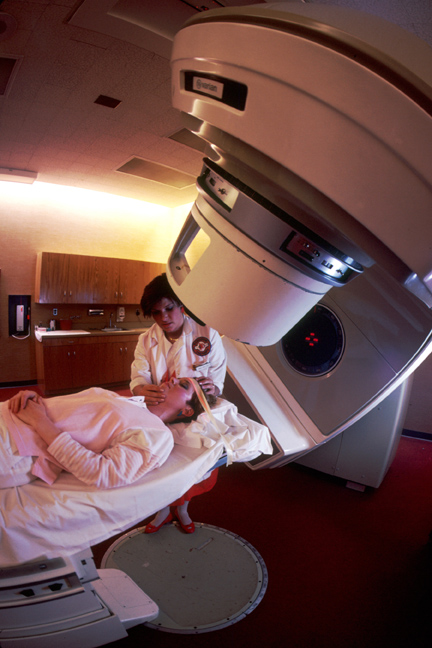
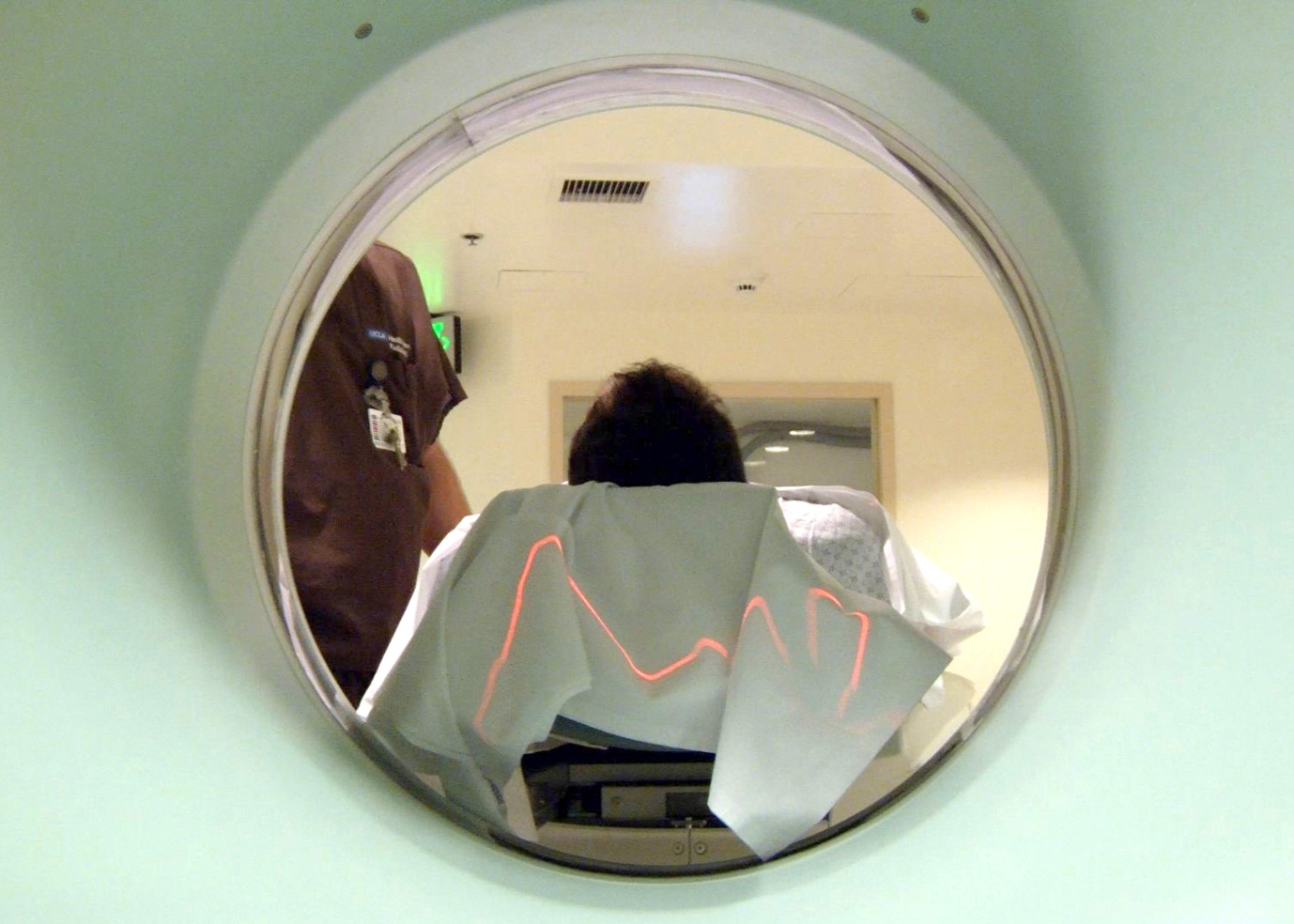
|
Radiotherapy: The idea for radiation therapy was developed over 100 years ago. Today radiotherapy is the most common treatment for cancer. Image credit: US National Cancer institute |
New radiotherapy techniques being developed that use particle accelerators, such as proton therapy, show clear signs of reducing side effects due to a reduction of the radiation dose in healthy tissues and for some types of cancer an increase in the possibility of curing the cancer; see section below on proton beam therapy.
For more information see:
Web: ESTRO, the European SocieTy for Radiotherapy and Oncology
Web (NHS): Radiotherapy
Web (National Cancer Institute): Radiotherapy factsheet
Electron beam therapy
This technique uses the same type of accelerator that is used to generate X-rays, however the X-ray producing target is removed so that the electrons are fired directly into the tumour. Electron beam therapy is useful for treating tumours near the surface of the skin as the electrons quickly lose their energy when they interact with atoms in the body (see the graph below). Electron beam therapy causes far less damage to healthy tissue in the body as the beam does not pass all the way through the body.
For more information see:
Lecture [2008]: Electron Beam Therapy Dosimetry, Planning & Techniques
Hadron beam therapy
A hadron is a type of particle made up of quarks. Hadron therapy falls into three categories:
- proton therapy
- neutron therapy
- ion (e.g. Carbon or Helium Ion) therapy.
The three types of hadron therapy differ in the type of particle beam that is used in the treatment. The dose deposition and its biological consequences depend on the particle type and its energy. The different therapies are used to treat different forms of cancer at different locations in the body as the particles penetrate and deposit their energy in different ways.
|
Gantry, the first and only compact scanning facility for the treatment of deep seated tumours using a scanned proton beam, has been operated at the Paul Scherrer Institute (PSI) in Switzerland. Patient treatments started at the facility in 1996. Image credit: Paul Scherrer Institute |
The dose deposition of high energy neutrons is much like that of X-rays. The therapeutic difference is the stronger biological effect (cell killing per amount of deposited dose) of neutrons. For a limited amount of cancers and at certain locations in the body, this can be of an advantage.
The advantage of proton and ion-beam therapy over current X-ray radiotherapy is that the particles do not penetrate the whole body; they are fired into the body with a certain energy which dictates the range of the particles. The range is the depth that the protons or ions can penetrate into the body. Once protons or ions reach this depth they stop, whereas X-ray radiation passes through the whole body, thus also damaging cells on the way in and on the way out. Using protons or ions, this means that, for a certain dose in the tumour, the patient is exposed to less radiation in regions outside the tumour and therefore less healthy tissue is damaged in the treatment.
Ions such as carbon have a larger biological effect than protons. This can be exploited in certain cases. But to accelerate ions to sufficient energies, much larger accelerators, beam transport systems and gantries are needed than for protons. Until the 1990s proton therapy was performed in nuclear physics laboratories that were equipped with a particle accelerator and in this period most of the pioneering proton therapy research was performed and most of the dose delivery concepts were developed.
For more information on hadron therapy in general see;
Web: PTCOG, Particle Therapy Co-Operative Group
Video: Particle Accelerators for Tumour Therapy [UK], 5min26s
Article [2011] (CERN Courier): Hadron Therapy Collaborating for the Future
Article [2010] (CNRS): Hadron Therapy, a Treatment for X-Ray Resistant Cancers
Book: Reviews of Accelerator Science and Technology, Vol. 2: Medical Applications of Accelerators (2009), (ed A. W Chao, W. Chou), World Scientific Publishing Company
Book: Proton Therapy Physics (ed H. Paganetti), CRC Press, Taylor & Francis Group, 2012
Book: Proton and Carbon Ion Therapy (ed C. Ma and A. Lomax), CRC Press, Taylor & Francis Group, 2013
For more information on proton treatment see;
Web (PSI): Proton Therapy at PSI
Web: CATANA, The First Italian Protontherapy Center for the ocular melanoma treatment
Article [2011] (Fermilab Today): Advancements in Proton Therapy Cause for Celebration
Article [2008] (Symmetry Magazine): The Power of Proton Therapy
Article [2012] (Medical Physics Web): Future Prospects for Proton Therapy
For more information on neutron therapy
Article [2005] (Symmetry Magazine): Neutrons for Cancer Treatment
Lecture [2012] (Fermilab): Fighting Cancer with Neutrons
For more information on heavy ion therapy
Article [2011] (Symmetry Magazine): Kicking Cancer with Carbon Ions
Web: Carboniontherapy.org
Web: CNAO Foundation, National Centre of Oncology in Italy
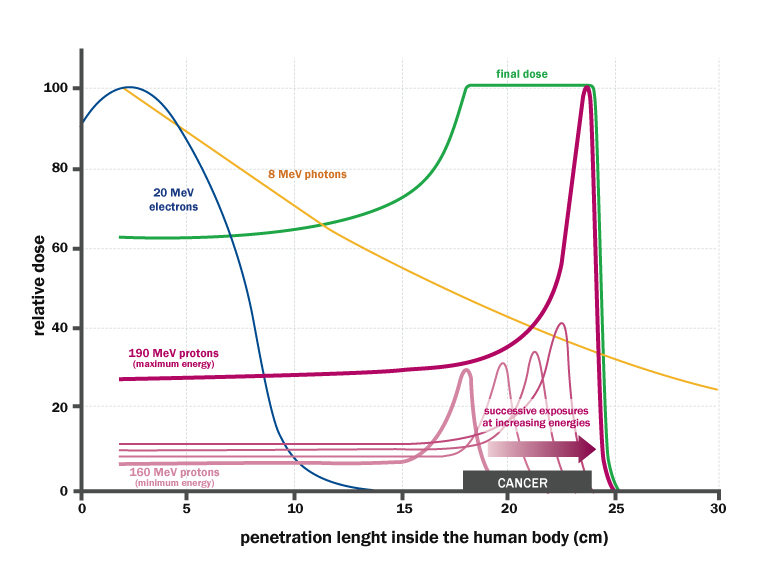
Relationship between different kinds of particles (at a given energy) and their ability to penetrate inside the human body : In depth distribution of the absorbed dose, in the case of 20 MeV electrons, 8 MeV photons, 190 MeV protons: Electrons and photons mainly affect the first layers of tissue, while protons release most of the energy to a precise depth, variable with the beam energy. The green line shows the distribution of the dose received by the patient in the case of treatment of a tumor with a thickness of 6 cm and located between 18 and 24 cm depth, irradiated with proton beams with controlled different energies. The dose is concentrated along the lesion, with limited damage to the surrounding tissues. Image credit: INFN/Asimmetrie, page 21.
Cancer research
Accelerator scientists are working on developing new techniques, such as a novel technique using synchrotron radiation from the ALICE accelerator at Daresbury Laboratory in the UK, to detect certain cancers early, refine earlier techniques and improve accelerator technology so that treatments like proton therapy can become economically accessible for more hospitals around the world.
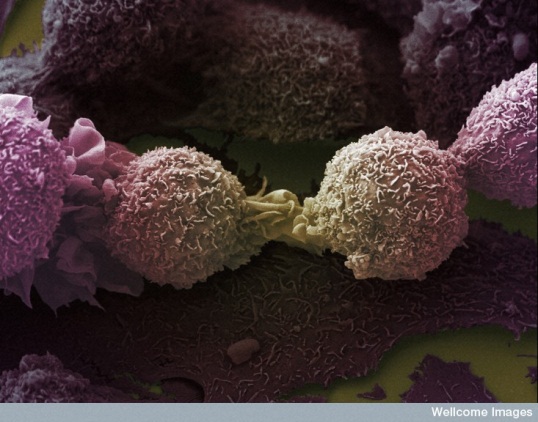
|
Cancer Research: Due to the numerous forms that cancer can take and the many treatments cancer research is a large and extremely important area of medical research. Image credit: Anne Weston, LRI, CRUK - Wellcome Images |
For more information see;
Article [2012] (Symmetry Magazine): Accelerator Beams for Early Cancer Detection
Article [2009] (Symmetry Magazine): Shrinking the Cost of Zapping Cancer
Article [2010] (Symmetry Magazine): Accelerator Physicists Strive to Lower Cost of Cancer Treatment
Article [2011] (Symmetry Magazine): SLAC Physicists Using Physics Simulation Tool to Make Cancer Therapy Safer
Article [2013] (STFC): Breakthrough in the Development of a Diagnostic test for Oesophageal Cancer
Medical Imaging
Medical imaging is an incredibly important area of medicine with applications in both diagnosis and research. Most of us will have an image of some part of our body taken for diagnosis in our lifetime, whether it is an X-ray image of our teeth at the dentist’s or a full body Magnetic resonance imaging (MRI) scan. The role of accelerators directly (as an X-ray source for radiography) and indirectly (in the development of the physical principles behind MRI imaging) on the development of new imaging techniques cannot be overstated.
Positron Emission Tomography (PET)
Positron Emission Tomography (PET) is a medical imaging technique which produces a detailed 3D image. A radioactive isotope is introduced to the body. The isotope undergoes radioactive decay within the body which emits a positron. As this particle travels through the body, it interacts with other particles in the body and slows to the point where it can annihilate with an electron producing a pair of gamma photons. These photons are then picked up by a detector which will send the data to a computer for the production of an image of the photon origins.
The physics behind this technique was first understood by particle physicists who also played a role in the development of the technique. The detectors used by PET scanners were developed first for particle physics experiments. Particle accelerators are also used in the synthesis of the radioisotopes used in this technique; this is discussed in the ‘Accelerators for Isotope Production’ section below.
PET scans can be combined with an MRI or Computerised Tomography (CT) scan to help make the images easier to interpret. A PET scan measures important body functions, such as blood flow, oxygen use, and sugar (glucose) metabolism, while CT imaging provides excellent anatomic information. The PET technique has the advantage of the use of atoms (PET isotopes) that are typical in biology, e.g.: carbon, oxygen, nitrogen and Fluor. It is also possible to determine the concentration of the isotopes in the 3D image in an absolute way, this makes the PET technique very powerful in many applications.
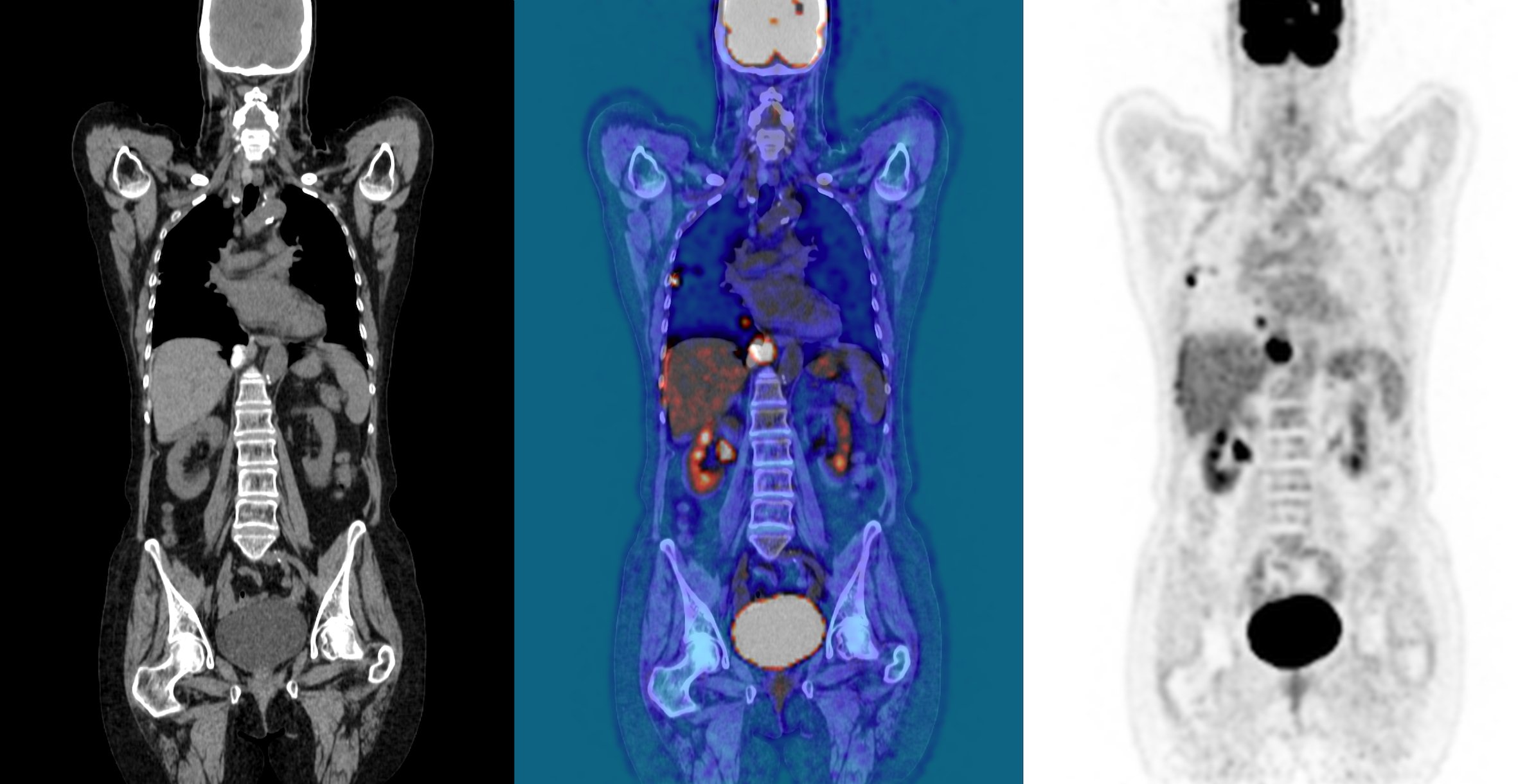 |
PET/CT imaging: At right is a CT scan, at left is a PET scan, at center is a combined PET/CT scan. Image credit: John Prior, CHUV, Switzerland |
For more information see;
Proton Computerised Tomography (CT) scan
Particle physicists and medical researchers are working together to develop a new medical imaging technique called a proton computerised tomography (pCT) scan, which is like a conventional computerised tomography (CT) scan but uses protons rather than X-rays. This new technique will reduce the patient’s exposure to harmful radiation whilst producing more accurate 3D images than those produced by current CT scans. A pCT scan also has great potential in improving the effectiveness of proton beam therapy which could improve proton therapy, and reduce side effects related to still existing range uncertainties of the proton beam.
|
Safer Imaging: Proton CT scans expose the patient to less, harmful radiation and produce a more accurate 3D image - Image credit: Public Policy Productions |
For more information see;
Article [2012] (Symmetry Magazine): Pursuing Protons for Medical Imaging
Article [2011] (Science Daily): Proton Imaging Provides More Accuracy, Less Radiation to Paediatric Cancer Patients
Article [2012] (University of California Santa Cruz): Image of Hand Shows Progress Towards Proton Radiography
Article [2010] (Northern Illinois University): Proton Centre on Verge of Major Medical Breakthrough
Magnetic Resonance Imaging (MRI)
Since its development in the 1970’s magnetic resonance imaging (MRI) scanning has saved countless lives due to its revolutionary ability to image soft tissue within the body. The basic physical principles were first discovered by particle physicists in the 1930’s and later the field of particle physics played another crucial role in the development of the powerful superconducting magnets required for the technique to work.
|
MRI an Accelerator Born Technology: Above is a still image from a GIF produced by artist Andy Ellison of an MRI scan of a husk of corn. Image credit: Andy Ellison |
For more information see;
Article [2008] (Symmetry Magazine): Deconstruction: MRI
Medical Materials Produced with Accelerators
Particle accelerators have become an important tool in the production of customised materials for industry (see section on industrial applications). The medical industry is no exception. Indeed specialized materials such as prosthetic implants or hydrogels are often produced using accelerators.
Heart valves
Bombarding materials with ions can produce materials with desirable properties. This technique has been used by scientists in the USA to produce a durable material to be used in artificial heart valves.
For more information see;
Article [2009] (Symmetry Magazine): Heart Valves
Hydrogels
Particle accelerators firing beams of electrons play an important role in the production of materials known as hydrogels. Hydrogels are used to make dressings for wounds like burns which are more comfortable for the patient than standard bandages and can be used in drug delivery.
 |
Hydrogels: Particle accelerators play a vital role in producing hydrogels for use in medicine. Image credit: Kathy F. Atkinson, University of Delaware |
For more information see;
Article [2010] (Symmetry Magazine): Hydrogels
Accelerators for Isotope Production
Scientists have found many uses for radioactive isotopes, notably in medicine where they can be used in medical imaging and radiotherapy.
A particle accelerator is used to produce isotopes by accelerating protons or other ions to close to the speed of light and smashing them into atoms to initiate a nuclear reaction, in which radioactive isotopes are produced. In a chemical process, these isotopes are included into molecules that can be brought into the patient’s body by e.g. inhalation, orally or by an injection. These molecules are used in specific processes in the patient’s body. The emitted radiation can be detected with special detectors and the obtained 3D image of the spread of the molecule then gives interesting diagnostic information. Apart from this diagnostic application, there is also a therapeutic application of radioactive isotopes. Isotopes that emit radiation with a very short range can be used to irradiate tissue, for e.g. the treatment of certain types of cancer.
|
Manmade Isotopes: Artificial isotopes made using accelerators play an important role in both medical imaging and radio therapy - Image credit: TRIUMF |
For more information see:
Article (from CERN Courier): Medical-isotope cyclotron designs go full circle
Article (from Symmetry): Radioisotopes
Doc (LANL): Accelerator Radioisotopes Save Lives
Lecture (isotope.gov): Medical Isotope Production and Use
Doc (IAEA): Cyclotron Produced Radionuclides: Physical Characteristics and Production Methods
![]() Video [US]: Isotope Cancer Treatment Research at LANL
Video [US]: Isotope Cancer Treatment Research at LANL
2min32s
See also in prospects, section on replacing ageing research reactors.
Further Reading / Watching
![]() Video: Physics for Health in Europe
Video: Physics for Health in Europe
2hr14min06s
Article [2011] (Symmetry Magazine): A Physicist in the Cancer Lab
Article [2007] (Symmetry Magazine): Commentary - Timothy Antaya